N3.Healthcare
Healthcare information systems integration based on HL7 FHIR
We build infrastructure for safe health information
exchange across regional and institutional boundaries
N3.Healthcare connects information systems that serve over 36 million patients
What is N3.Healthcare?
N3.Healthcare is an E-health integration platform that connects healthcare information systems through application programming interfaces (API) based on HL7 FHIR to exchange information about patients. We support CDA, HL7 v2&v3.
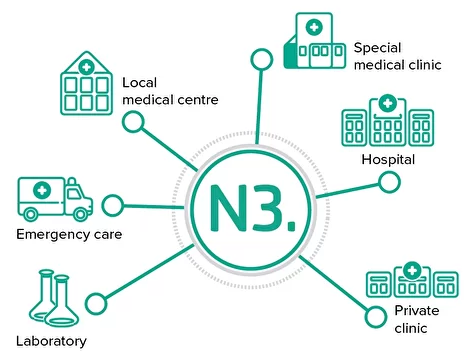
How can N3.Healthcare help?
Large hospitals all over the world are facing unprecedented IT challenges. It is not uncommon for a hospital to operate a couple of dozens of various systems. Choosing the right architecture to manage a proliferating IT ecosystem is a cornerstone to profitability and sustainable growth.
Expand your EHR
You can overcome the shortages of your current EHR by adding additional specialized services from other vendors. We connect health information systems via an HL7 FHIR interface so that any types of data can be accessed from EHR or HIS currently used in your hospital.
Save money on integration
When you implement N3.Healthcare integration platform you get a single integration point that provides API to other systems and unified information exchange rules for all. No more need for point-to-point integration.
Single point of authorization for medical staff
In some organizations doctors have to remember several dozens of logins and passwords to do their day-to-day work. With N3.Healthcare in place, you get a single authorization point, simple and secure access procedures.
Grow your partner network
You can grant access to your data to trusted external institutions such as partnering clinics. Authorization rules and data access policies powerd by XACML-based data security module.
Simplify access and protect data
N3.Data security module is a single and secure point of authorization for medical staff and other users. You can flexibly manage data access policies and grant access up to a specific item - a type of document or a specific health entry. Patients can access their data at the Patient's portal view medical records, lab results, scheduled appointments and more.
Harmonize terminology across systems
Data normalization across departments and automated mapping help overcome the problems associated with employing multiple, incompatible medical terminologies. Avoid incostincencies, eliminate excel spreadsheets and time-consuming meetings.
About company
Services
Leave your contacts to request a demo
Contact us
- Phone 007 (812) 500 98 01
- E-mail: zs@n3med.ru
- Address: St.Petersburg, Russia, 191015, Furazhny per. 3 lit K